ScoliScan Radiation-Free Scanning FAQs – Part 1
What is the scanner?
The DIERS Formetric Scanner (ScoliScan) was originally invented in Germany and has been developed over the last 25 years with the objective of reducing the x-ray radiation dose on patients being followed for scoliosis and developing a procedure which offers a replacement for x-rays in some cases. The scanner has been in use in its current model across Europe and Asia for the past 10 years. The scanner recently received FDA approval for use in the United States and only a few scanners are currently available here. The scanner provides a unique optical measurement of the back and spine like no other diagnostic assessment currently available in the world.

How does the scanner work and what is a scan like?
The scanner itself consists of a camera, a light source, a computer and a foot simulation platform. The scanner is operated by a technician who sets up the positioning of the patient and the camera to ensure that the resulting image is accurate.
The patient stands a few feet away from the camera, with their back facing the camera and light source and their feet planted on the simulation platform. The scan takes only 6 seconds, during which the light source projects harmless white light beams horizontally across the patient’s back. These light beams allow the computer to measure the high and low points of a patient’s back shape, from the top to the base of the spine and across their back. Immediately afterwards, the computer is able to use the information gathered during the scan to reconstruct a 3D image of the patient’s spine. The computer also takes information about the patient’s feet from the platform, including possible leg length differences and foot malpositions.
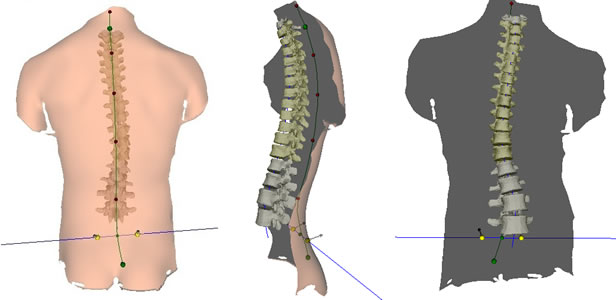
What do the results look like? How are the results used?
The image is immediately visible to the patient and the physician after the scan and can be analyzed by Dr. Lonner to make clinical determinations about the patients’ care. The image can also be compared to standard AP and Lateral x-rays taken, in order to have a complete clinical picture of the patient’s deformity. The computer creates a report which provides images and information about the curve of the patient’s spine (curves visible both straight on and from the side), the angle of pelvic tilt, the rotation of the chest cavity, leg length differences, uneven hips and much more. The image of the spine is also very realistic, and therefore easy for the patient to understand as well.
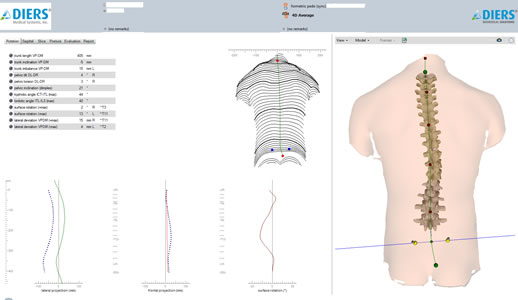
Since the scan provides Dr. Lonner with a 3D image of the patient’s spine, he can get a more accurate picture of the patient’s deformity globally, or how the deformity looks from all angles. This is not possible with a 2D X-Ray.
Especially for patients with severe curves, the effects these curves have on other aspects of one’s truncal alignment, or shape of their trunk, are best seen with the 3D scanner’s 360° images. Also, unlike x-rays, the accuracy of the scan does not depend on patient positioning and when done over time, can be used as the standard assessment tool for the patient’s progress.
Dr. Lonner can use the measurements and images from the scan to diagnose a new patient, but also to follow-up with past patients who may have had surgery or whose condition has not progressed, and therefore x-rays are not mandatory.
