COMPREHENSIVE APPROACH to NON-SURGICAL SCOLIOSIS AND KYPHOSIS CARE
The most important element of non-operative scoliosis and/or kyphosis care isn’t a brace; it is the patient.
Conservative treatment relies heavily on a patient’s compliance, honesty and vigilance, and we are here to educate and empower you. We encourage active participation in your treatment plan as a member of a multidisciplinary team that includes YOU, your family, your physician, orthotist, physical therapist, and counselor if necessary.

Upon visiting our practice to have your spine evaluated, we will collect information regarding your medical history, perform a physical exam, and obtain diagnostic images (X-rays and/or Scoliscan). With this information, a decision can be made on how to proceed with caring for your spine and body.
Currently, standard imaging of the spine is done by x-ray. However, we have been leaders in the use of non-xray, light-based surface topography screening (Scoliscan). Ask our team about Scoliscan and whether you or your child is a candidate for this imaging tool. Please note, though it is not covered by insurance, we have priced it reasonably to give our patients access to this special and safe technology.
Small scoliosis curves less than 20 degrees, or curvatures up to 40 degrees in skeletally mature (reached end of growth) patients, do not require bracing or surgery. Nor do mild cases of kyphosis (round back). Therefore, observation is the standard of care if your curve measurement is low, and your curve isn’t progressing or causing pain. If observation is right for you, we will set up a program for you to visit us periodically. Physical therapy and home exercise may also be prescribed. We will monitor (observe) your curve by means of physical exam and imaging. If changes are noted at subsequent visits, we may collaboratively change your treatment plan. This may include the need for bracing or potentially surgery.

There has been a movement in recent years toward the use of specific exercise and physical therapy programs directed toward the treatment of scoliosis. Although the highest level of clinical evidence is still lacking for these techniques, we do believe that exercise and physical activity in many forms are useful in helping patients with postural realignment, decreasing muscle fatigue and discomfort, and improving breathing mechanics. To date, little evidence exists that curve progression can actually be stopped with exercise and/or physical therapy methods alone, but clinical trials are ongoing that hope to answer this question.
The Schroth Method is a physical therapy technique developed in the 1920s specifically for scoliosis. Its thesis states, “scoliosis involves asymmetrical muscle groups in the back and elsewhere, which in normal bodies are more evenly symmetrical.” The method, therefore, consists of exercises meant to strengthen certain muscles around the spine and within the torso while stretching and lengthening others. Its goals are to reverse abnormal curvatures and associated pain. Schroth Method exercises are coordinated in three dimensions, sagittal (side), frontal (side to side), and transverse (cross sectional). They include breathing techniques, pelvic corrections, isometric contractions, and posture practices. Therapy is tailored to the individual. The aim is to teach the patient about his or her own body, and demonstrate practices that can be implemented in daily life rather than just during exercise sessions. We have certified Schroth therapists available at our Manhattan location who can be contacted for an appointment.
While physical activity and formal exercise are important in everyone’s daily life, exercise is especially important for patients who have scoliosis and/or kyphosis. Exercise strengthens the muscles of the back and abdomen (the so-called core), thereby decreasing episodes of back pain throughout your life and improving your ability to carry out your daily activities including sports and exercise.

PEDIATRIC / ADOLESCENT PATIENTS
If your scoliosis curve measures between 20-40 degrees or your kyphosis (roundback) curve measures greater than 50 degrees, and you are still growing, our team may prescribe a brace. Bracing your spine may achieve one or both of the following:
*Bracing may also address body alignment issues, such as a shift of the upper body to one side, or uneven shoulder levels. It may also improve a rib prominence (bump) through molding of the chest wall.
The brace is worn until growth is completed. We monitor growth by using skeletal x-rays to evaluate four growth centers: the femur, iliac crest, humerus and ribs. Once skeletal maturity is reached, these growth centers close. On average, girls complete their growth at age 15-17, by two years post menarche (the first menstrual period). Boys complete their growth by age 16-19 years, on average.
You are to wear the brace 16-23 hours per day depending on the severity of the curve and how much growth remains. A more precise number, tailored to your needs, will be discussed with our team. Time in brace: The brace can be worn to school, to bed, and for almost all daily activities. It may be
The brace can be worn to school, to bed, and for almost all daily activities. It may be worn for gym and non-contact sports, or you can take the brace off for these activities and count that among your “out of brace” time. The brace should not be worn for contact sports.
Patients are encouraged to do core strengthening exercises (sit-ups, yoga, Pilates, swimming), if not participating in active sports or gym, while they are out of the brace. It may be removed for after-school sports. Additional latitude is given during the summer to allow for camp activities. Swimming is an excellent activity for your back.
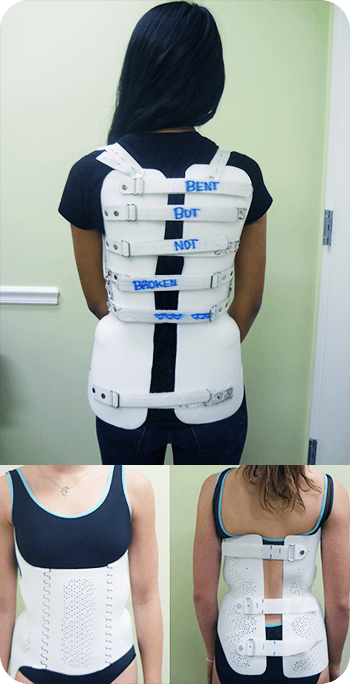
What are the types of braces?
There are various types of scoliosis braces available to patients. Our practice is committed to providing patients with the most innovative technology to improve results.
ADULT PATIENTS
Brace wear in adult patients may be useful, but for different reasons than pediatric or adolescent patients. In adults, a spinal deformity will not be halted or corrected by use of a brace, because the bones have completed growth. Bracing in this population is intended for support and pain reduction purposes only, and is part of a comprehensive non-operative program that should include exercise and close observation. It is important to combine bracing with exercise so that your core is not deconditioned due to the unloading of muscles during physical activity. Dynamic bracing using a strap system (SpineCor) may be helpful for some adults.This can be discussed with our team.
A brace can only serve its purpose if it fits well and is worn for the number of hours prescribed, and we strive to make those objectives as attainable as possible. We will facilitate choosing a brace type to suit your individual needs and preferences.
The BRAIST Study
In 2013, the Bracing in Adolescent Idiopathic Scoliosis Trial (BRAIST) study was published in the New England Journal of Medicine. This study was significant in determining the effectiveness of bracing, as compared with observation, in prevention of curve progression to 50 degrees or a recommendation for surgery.
Twenty five institutions throughout the US and Canada collected data on 242 patients who had curves for which bracing was indicated (20-40 degrees). The participants were aged 10-15 years old, and had Risser scores of 0-2 (indicating growth was not yet complete). One hundred forty six patients wore braces for the study, while 96 were observed only for curve progression.
Patients who wore braces used the thoracolumbosacral orthotic (TLSO) type most commonly utilized in their institution’s clinical practice; most wore Boston style braces. They were instructed to wear their braces for a minimum of 18 hours/day, and a temperature logging tool within the brace confirmed compliance with these instructions. Patients were evaluated, including x-ray, every 6 months during the study.
Bracing success was defined as reaching skeletal maturity (the end of growth) without progression to a 50 degree curve. Failure was defined as curve progression to 50 degrees and/or recommendation for surgery. Seventy-two percent of patients who wore a brace were considered successful, while only 48% of patients who were observed without wearing a brace had a successful outcome.
Additionally, the amount of time the patient wore a brace correlated with the rate of success. Patients who wore their brace for 0-6 hours per day had only 41% success. This was similar to the results of those who were observed without wearing a brace. Meanwhile, those who wore their braces for 18 hours per day, as instructed, had a success rate of 90-93%.
The BRAIST study provides strong support for the conclusion that bracing reduces the risk of curve progression and need for surgery. It also shows the importance of wearing a brace for the prescribed number of hours per day. You can read the study itself at http://www.nejm.org/doi/full/10.1056/NEJMoa1307337
