Ehlers-Danlos Syndrome
People with Ehlers-Danlos syndrome have abnormalities in the synthesis, processing, and structure of collagen, which is one of the main structural proteins in the human body. Collagen is a relatively rigid substance that gives tissue strength, elasticity, and firmness. Because of collagen's important role throughout the body, people with Ehlers-Danlos syndrome may have symptoms that impact the blood vessels, ligaments, joints, skin, intestines, or uterus.
Types of Ehlers-Danlos syndrome
Historically there were ten types of Ehlers-Danlos syndrome, but current naming includes only six major types:
- Classic (EDS types I and II)
- Hypermobility (EDS type III)
- Vascular (EDS type IV)
- Kyphoscoliosis (EDS type VI)
- Arthrochalasia (EDS type VIIA and B)
- Dermatosparaxis (EDS type VIIC)
While there are some clinical features of that overlap between these types, certain symptoms and abnormalities are unique to the specific condition. Skeletal and joint abnormalities can occur in all of these forms of Ehlers-Danlos syndrome.
Symptoms
Ehlers-Danlos syndrome generally causes loose, fragile skin and tendons and hypermobile (“bendy”) joints. Often these abnormalities result in pain, bruising, tearing, and joint dislocation. Pain can range from mild to severe.
Collagen is a key component in blood vessels that helps strengthen them against rupture, so Ehlers-Danlos syndrome causes frequent arterial ruptures and prevalent varicose veins. Individuals with Ehlers-Danlos syndrome who become pregnant can undergo severe complications, including premature membrane rupture, uterine tearing, and unusually heavy bleeding during childbirth.
The effect of Ehlers-Danlos syndrome on bone and joints
Ehlers-Danlos syndrome has specific consequences relating to development of the skeletal system. Since joints are stabilized by cartilage that is partially composed of collagen, individuals with Ehlers-Danlos syndrome often suffer dislocations or sprains of the joints. Early onset of advanced osteoarthritis is common due to the breakdown of these joints. Moreover, the breakdown of joint cartilage lessens its ability to cushion bones and ligaments, resulting in splintered bones, fractures, or ligament strain. Complex bone systems, such as the hands and feet, can develop deformities due to the instability of the joints.
Kyphoscoliosis, a deformity of the spine, is associated with EDS Type 6:
- Scoliosis, where the spine curves to the side
- Kyphosis, where the spine forms a hump in the upper back
- Severely limited spinal movement, which can damage the spinal cord in some cases
Arthrochalasia EDS (EDS VIIA, VIIB) results in joint hypermobility with recurrent subluxations, hip dislocations starting at birth, muscle contractures in the limbs, scoliosis and subsequent short stature, poor muscle tone, and frequent bone fractures.
Treatment
There is no cure for Ehlers-Danlos syndrome, but with proper care, patients can minimize their risk and manage pain and other symptoms. One of the best treatments for the disease is to take preventative steps to avoid injury. Many patients are prescribed supplements to encourage skin and tendon healing. Likewise, every patient should be counseled on which activities can aggravate their condition and cause injury. Patients should closely monitor their cardiovascular risk factors and undergo frequent monitoring to rule out aneurysms or outpuchings of the blood vessels.
The magnitude of pain and symptoms varies from person to person, so the level of managed care needs to be tailored to the individual. Physical therapy aims to improve strength of muscles surrounding a joint, thereby stabilizing the area and preventing dislocations.
Kyphoscoliosis in Ehlers-Danlos syndrome is best managed by an orthopedic surgeon, specifically an orthopedic surgeon with specialization in scoliosis. Bracing may be helpful in some patients to prevent curve progression or worsening. In some cases, orthopedic surgery is required to correct the scoliosis.
Patient Story
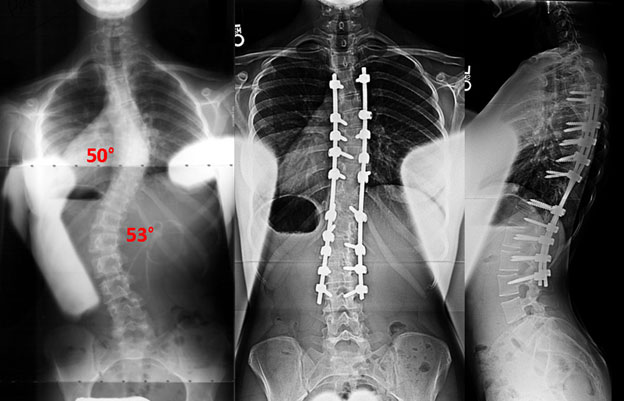
This is a 15-year old girl with has scoliosis and Ehler’s-Danlos syndrome. Her major curve progressed from 44° to 53° in 4 months, despite the prior 2½ years of brace treatment. Dr. Lonner performed a posterior (back) fusion and she has done very well, returning to full activities.
