Prader-Willi syndrome
Prader-Willi syndrome is a genetic disorder that affects about one person in 15,000. Men and women across all cultures are uniformly affected by the disorder. Symptoms arise from a modification or deletion of genes on chromosome 15 through spontaneous mutation or damage to the hypothalamus in childhood. Prader-Willi syndrome is diagnosed through genetic testing.
Symptoms of Prader-Willi syndrome
Specific physical and mental changes
Prader-Willi syndrome can be recognized by the presence of certain facial features, including almond-shaped eyes, a thin upper lip, a prominent nasal bridge, and a high, narrow forehead. People with this condition often exhibit decreased muscle tone, short stature, behavioral and cognitive problems, and incomplete sexual development.
Increased pain tolerance
Individuals with Prader-Willi syndrome also have a high pain tolerance. This means that individuals with the syndrome may present to health care providers with very advanced conditions. For example, a case of appendicitis is first recognized by someone as abdominal pain. In people with Prader-Willi syndrome, they do not recognize the abdominal pain until the bowel inflammation is very advanced. This can lead to serious complications.
Increased appetite and decreased muscle tone
The most notable symptom of Prader-Willi syndrome, for many, is an unusually large, seemingly insatiable appetite. Low muscle tone results in physical weakness, and infants often have trouble feeding due to weakness in muscles that allow sucking. This tendency is markedly changed in early childhood into adulthood, when patients experience insatiable hunger and overeating. Because of the large appetites and slowed metabolism that are characteristic of Prader-Willi syndrome, sufferers are often overweight or obese. In fact, Prader-Willi syndrome is the most common cause of genetic morbid obesity in children.
The effects of Prader-Willi syndrome on bone
Along with lack of muscle development, people with Prader-Willi syndrome also have lower bone density than their healthy peers. Low bone density can lead to fractures. When fractures occur in the spine, the spine can take on an abnormal shape such as a rounded back.
Growth hormone injections can minimize bone density loss and may be used in conjunction with proper nutrition to ensure that the individual is getting enough vitamin D and calcium. Likewise, properly timed administration of sex hormones such as estrogen, progesterone, or testosterone can help foster sexual maturation and development.
A focus on scoliosis in Prader-Willi syndrome
Scoliosis emerges in Prader-Willi syndrome in two age ranges, under the age of 4 and around 10 years of age. Younger children have C-shaped scoliosis, which results from poor muscle tone. The older group has S-shaped scoliosis, typically. Children with Prader-Willi syndrome should have routine monitoring for scoliosis starting when the infant can sit independently. This monitoring includes yearly clinical visits and spine radiographs (X-rays) as needed. If the spine shows signs of abnormal bending during these screening visits, X-rays may be needed more frequently.
Treatment
A wider variety of treatments are becoming available for those with Prader-Willi syndrome, and most individuals with the disorder are able to live happy, fulfilling lives with hormone injections, physical therapy, and other interventions. Growth hormone injections during childhood can help improve physical development by improving muscle mass. These injections may be limited if they exacerbate appetite and weight gain.
Pharmaceutical weight loss aids are not recommended, as they have not been shown to effectively control appetite or reduce binge eating. On the other hand, psychotropic drugs can mitigate overeating in some individuals. Weight loss surgery has been shown to be effective in some cases, though it usually only used when behavioral methods have been proven ineffective.
Because of decreased muscle tone and increased body weight, sleep apnea is common among children with Prader-Willi syndrome. This can be managed with a positive airway pressure machine (i.e., CPAP).
Scoliosis treatment
Because of the unique nature of the condition, patients with Prader-Willi syndrome should be followed by and cared for by an orthopedic surgeon, particularly someone with experience in scoliosis care.
Treatment of scoliosis can involve casting, bracing, physical therapy, and surgery. Scoliosis that is diagnosed in an infant (up to age 3) with Prader-Willi syndrome may be successfully treated by casting the spine.
Bracing, specifically a thoracic-lumbar-sacral orthosis or TLSO, is used to treat scoliosis in children older than three years of age. The TLSO is worn for 16-20 hours per day to be effective. The time in brace is reduced over time as the patient achieves skeletal (bone) maturity or the end of growth.
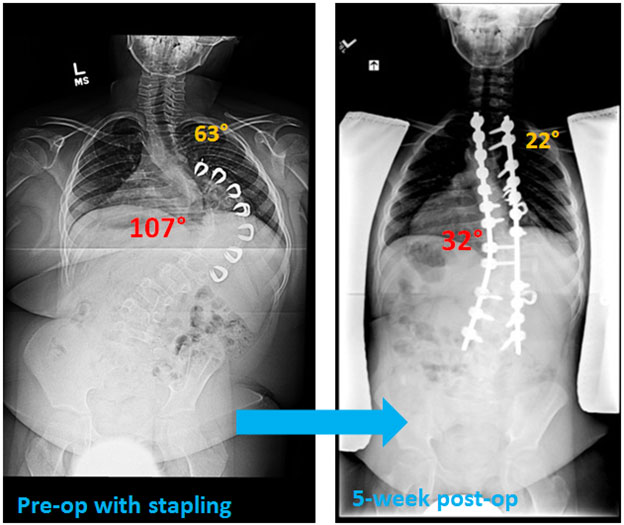
If the curvature of the spine exceeds about 40 to 50°, scoliosis surgery is required. Spinal fusion is a curative option for scoliosis, but in younger children (up to 10 years of age), the surgery could permanently restrict growth of the spine and chest. Alternatively, orthopedic surgeons can use expandable implants to correct spine curvature and permit bone growth. If these options fail, however, definitive spinal fusion surgery may be needed. Indeed, definitive spinal fusion is the treatment of choice in older children with Prader-Willi syndrome and scoliosis. Newer tethering procedures in which growth and motion are preserved can be offered to select patients.
Patient Story
Brennen is a 12-year-old young man with Prader-Willi syndrome and severe, progressive scoliosis. Despite multiple prior operations and bracing, his curvatures continued to progress. Dr. Lonner performed a final definitive operation to correct Brennen’s spine. Brennan has since resumed full activities and is a very active and inquisitive young man.
Dr. Lonner with Brennen at 5 weeks post-operative visit